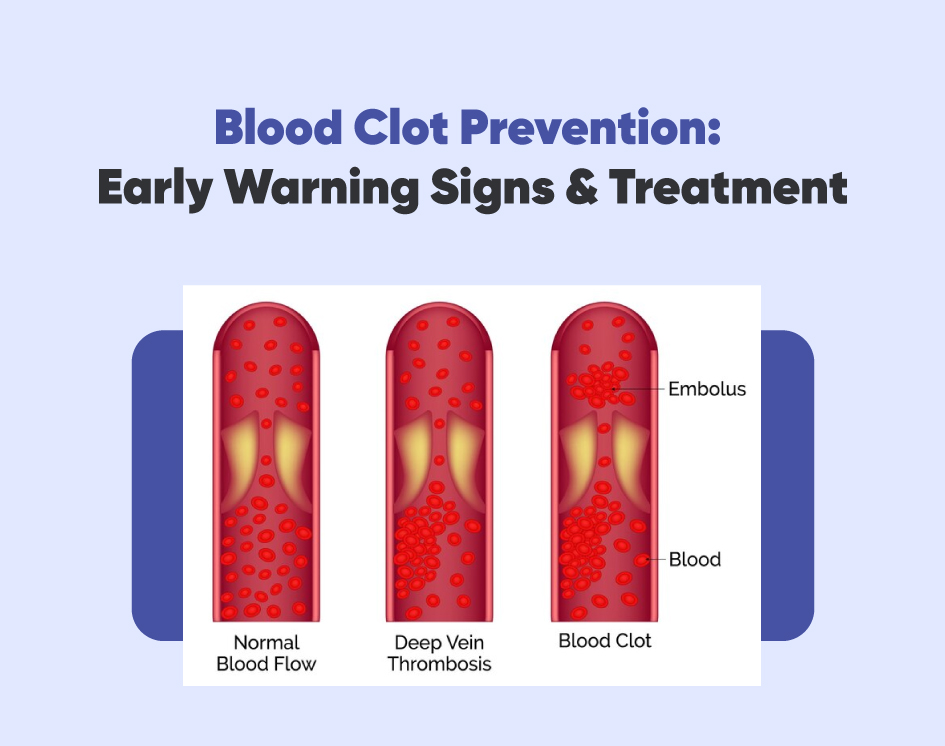
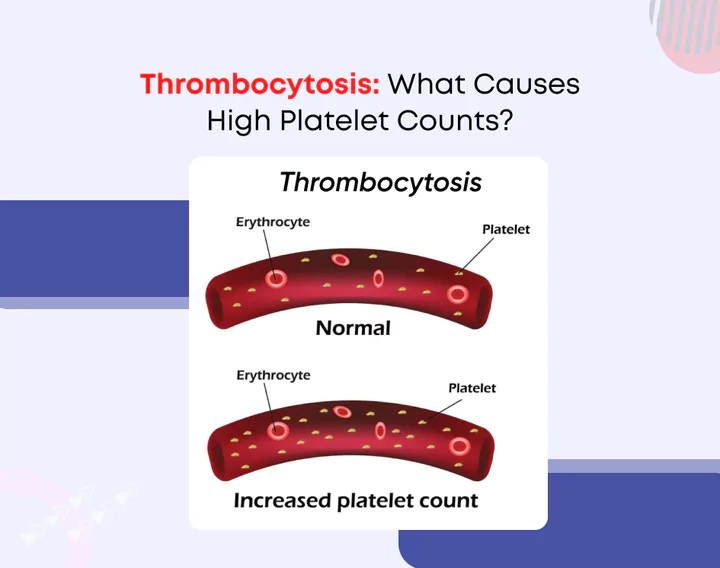
Blood thinning medications commonly called blood thinners play a critical role in preventing and treating blood clots that can lead to life-threatening conditions such as stroke, heart attack, deep vein thrombosis (DVT), and pulmonary embolism.
While these medicines are highly effective, they are not without risks. Understanding the side effects of blood thinners, especially in elderly patients, helps ensure safe and informed use.
What are blood thinning medications?
Blood thinners do not actually “thin” the blood. Instead, they reduce the blood’s ability to clot, lowering the risk of harmful clot formation.

Common categories include:
- Anticoagulants – prevent clot formation
(e.g., Warfarin, Heparin, Apixaban, Rivaroxaban, Dabigatran) - Antiplatelet drugs – prevent platelets from sticking together
(e.g., Aspirin, Clopidogrel)
These medications are commonly prescribed for:
- Blood clots in veins or lungs
- Irregular heart rhythms (like atrial fibrillation)
- Post-surgical clot prevention
- Heart disease and stroke prevention
How do blood thinners help with blood clots?
Blood thinners are essential for:
- Preventing existing clots from growing
- Reducing the risk of new clot formation
- Improving blood flow in patients with clotting disorders
However, because clotting is also a natural protective mechanism, excessive clot inhibition can increase bleeding risk.
Common Side Effects of Blood Thinning Medicines
Easy Bruising
Minor bumps may cause visible bruises due to reduced clotting ability.
Prolonged Bleeding
- Bleeding from cuts lasts longer
- Nosebleeds or gum bleeding may occur
- Minor injuries may bleed more than usual
Gastrointestinal Discomfort
Some patients experience:
- Nausea
- Indigestion
- Abdominal discomfort
This is more common with certain oral blood thinning pills.
Serious Side Effects of Blood Thinners
Internal Bleeding
This is the most serious risk and may occur in:
- Brain (intracranial bleeding)
- Stomach or intestines
- Urinary tract
Warning signs include:
- Black or bloody stools
- Blood in urine
- Severe headache or confusion
- Vomiting blood
- Sudden weakness or vision changes
Excessive Menstrual Bleeding
Women may notice heavier or prolonged periods.
Allergic Reactions (Rare)
- Rash or itching
- Swelling of lips or face
- Difficulty breathing
Immediate medical care is required in such cases.
Side Effects in Elderly Patients
Older adults are more vulnerable due to:
- Reduced kidney and liver function
- Higher risk of falls
- Multiple medications (drug interactions)
In elderly patients, blood thinner side effects may include:
- Increased risk of brain bleeding after minor trauma
- Severe anemia from unnoticed blood loss
- Dizziness or weakness
Close monitoring and dose adjustments are critical in this age group.
How do blood thinners and medication interact?
Blood thinning drugs can interact with:
- Painkillers (NSAIDs like ibuprofen)
- Certain antibiotics
- Herbal supplements (ginkgo, garlic, ginseng)
- Vitamin K–rich foods (for warfarin users)
Patients should never start or stop medications without medical guidance while on blood thinners.
How to reduce the risk of side effects?
- Take medicines exactly as prescribed
- Attend regular blood tests (INR monitoring if required)
- Inform doctors and dentists before procedures
- Avoid high-risk activities that may cause injury
- Report any unusual bleeding immediately
When to seek immediate medical attention?
Seek urgent care if you experience:
- Severe or uncontrolled bleeding
- Sudden headache or neurological symptoms
- Blood in vomit, stool, or urine
- Unexplained weakness or collapse
Early intervention can be lifesaving.
Conclusion
Blood thinning medications are life-saving drugs, but they require careful use, regular monitoring, and patient awareness.
If you are prescribed blood thinning medicine and notice unusual symptoms, do not ignore them. Prompt medical advice can prevent serious complications. Informed patients have safer outcomes.