Key Facts
- Nearly 50% of DVT cases show no clear symptoms.
- Pulmonary embolism can occur without leg pain.
- Ultrasound is the most common non-invasive test for DVT.
- Immediate testing is vital when symptoms are present.
Can I Check Myself for a Blood Clot?
You cannot confirm a blood clot at home, but you can watch for key warning signs. If you experience sudden leg swelling, pain, redness, or unexplained shortness of breath, you should seek medical attention immediately. Blood clots can be life-threatening if they travel to your lungs, brain, or heart.
Let’s help you understand how to recognize symptoms, what medical tests are used to detect clots, and when you should see a hematologist for blood health evaluation.
What Is a Blood Clot?
A blood clot forms when blood thickens and clumps together, usually as a normal response to injury. However, clots that form inside your veins or arteries without an injury can block blood flow, leading to serious health problems.
Venous thromboembolism (VTE) which includes deep vein thrombosis (DVT) and pulmonary embolism (PE) is one of the most common and dangerous clotting issues.
Types of Blood Clots
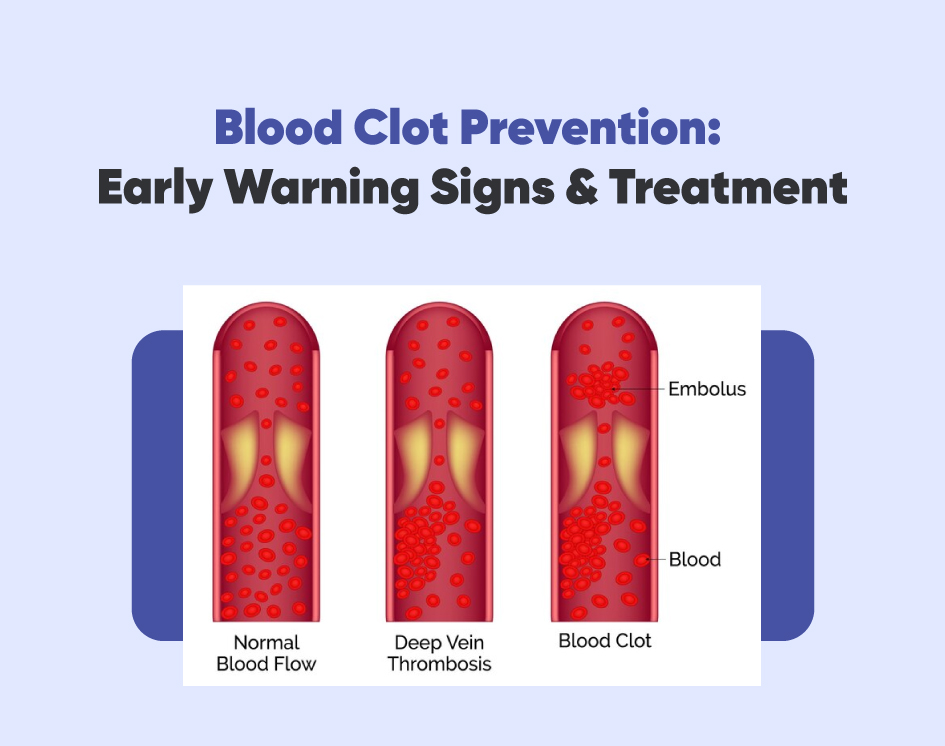
Deep Vein Thrombosis (DVT)
DVT occurs when a clot forms in a deep vein, often in the legs. It may cause swelling, pain, and redness.
Pulmonary Embolism (PE)
If a part of a DVT clot breaks loose, it can travel to the lungs and cause a PE, a medical emergency that can block oxygen supply.
Superficial Thrombophlebitis
This is a clot in a vein just under the skin. While less dangerous, it can signal an increased risk of deeper clots.
Arterial Clots
These clots can cause strokes or heart attacks and require immediate medical care.
Key Symptoms
Deep Vein Thrombosis (DVT):
- Swelling in one leg or arm (rarely both).
- Pain or tenderness, especially when walking or standing.
- Warmth or redness around the affected area.
- Visible surface veins or discoloration.
Pulmonary Embolism (PE):
- Sudden shortness of breath.
- Sharp chest pain that worsens when breathing deeply.
- Rapid heartbeat or palpitations.
- Coughing up blood.
- Lightheadedness or fainting.
Stroke or Arterial Clots:
- Sudden weakness or numbness on one side of the body.
- Trouble speaking or understanding speech.
- Sudden vision problems.
- Severe headache with no known cause.
When Symptoms Mean Emergency?
Call emergency services immediately if you experience:
- Severe difficulty breathing.
- Chest pain or pressure.
- Coughing blood.
- Sudden numbness or weakness (possible stroke).
- Fainting or collapsing.
Quick medical attention can save your life.
Who Is at Higher Risk for Blood Clots?
Some people are more likely to develop clots due to certain conditions or lifestyle factors:
- Recent surgery or hospitalization.
- Long periods of immobility (bed rest or long flights).
- Cancer or ongoing treatment.
- Pregnancy or postpartum period.
- Usage of hormonal contraceptives or hormone replacement therapy.
- History of blood clots or a family history of clotting disorders.
- Chronic health conditions like heart disease or infections.
- Smoking, obesity, or older age.
If you have multiple risk factors, regular blood health checkups with a hematologist are recommended.
How Do Doctors Check for Blood Clots?
Doctors use a step-by-step process to detect clots:
History & Physical Exam: Your symptoms, recent travel, surgeries, or family history are evaluated.
Risk Assessment: Tools like the Wells score are used to estimate the likelihood of a clot.
D-Dimer Test: A blood test that checks for clot breakdown products.
Imaging: Ultrasound for DVT or CT pulmonary angiography (CTPA) for suspected PE.
You cannot rely on symptoms alone. Imaging tests remain the definitive method for confirmation.
Diagnostic Tests Explained
D-Dimer Blood Test
This test detects fragments of blood clots present in your bloodstream. A normal (negative) result usually rules out DVT or PE in low-risk cases. However, a positive result does not necessarily confirm the presence of a clot.
Duplex/Compression Ultrasound
This is the first imaging test for suspected DVT. It checks if the vein compresses properly and measures blood flow.
CT Pulmonary Angiography (CTPA)
For suspected PE, this scan provides detailed images of the lung’s blood vessels.
Ventilation/Perfusion (V/Q) Scan
Used when CT scans are not suitable, such as in certain allergies or pregnancy.
MR Venography or Venography
Specialized tests used when ultrasound is inconclusive or to map complex clot locations.
Additional Blood Tests
Hematologists may order clotting profiles or genetic tests if you have unprovoked or recurrent clots.
Clinical Probability Tools
Doctors use specific tools to reduce unnecessary tests:
- Wells Score: Evaluates DVT/PE likelihood based on symptoms and history.
- PERC Rule: Helps rule out PE in very low-risk cases.
- Age-Adjusted D-Dimer: Prevents false positives in older patients.
What to expect at a hematology visit?
Your hematologist will:
- Review your personal and family clot history.
- Examine past imaging or lab results.
- Suggest further tests (like thrombophilia screening) if needed.
- Create a prevention or treatment plan, including blood thinners if required.
Prevention & Self-Monitoring Tips
- Stay active. Avoid sitting for long hours.
- Do simple leg exercises during long flights.
- Wear compression stockings if advised.
- Take prescribed anticoagulants exactly as directed.
- Stay hydrated and maintain a healthy weight.
- Report new swelling, pain, or shortness of breath immediately.
Final Word
Blood clots can be serious, but they are manageable with timely detection and appropriate treatment. If you notice unusual swelling, pain, or shortness of breath, don’t wait—get medical attention immediately. For personalized prevention and diagnosis, consult a hematologist.